
| Theme: 5AA Evaluation of the teacher | |||
 |
||||||
| Medical students experiences of and perspectives on role models |
 |
|||||
|
||||||
Role models (RM) are known to be a strong educational strategy. However, students learn from RM both consciously and unconsciously, and there is RM with undesirable behavior as professionals. The purpose of this study was to clarify medical students’ experiences and their perceptions of RMs.
To analyze medical students’ RM, 113 6th-year medical students in 2013 and 2014, who had finished the undergraduate medical program, completed a questionnaire asking about
- whether they observed
- good RM (positive RM)
- those who made them feel ‘I should not behave like that’ (negative RM)
- in terms of a) relationship with patients, b) clinical expertise,c) humanity, d) lifestyle, e) teaching, and f) community contribution.
- the frequency of certain clinical experiences.
- The majority of students had both positive and negative RM.
- They encountered more negative RM in terms of relationship with patients, humanity, and teaching than clinical competency and community contribution.
- Students’ recognition as ‘negative’ may indicate that a gap exists between students’ values and each doctor’s behavior and professional standard.
Students critically look at medical doctors’ attributes and behavior, including interpersonal skills and humanism.
This work was supported by JSPS KAKENHI (Grant Number 24590620).
The author gratefully acknowledges all participants who took part in this research, and specifically Kyoko Mineyama for her excellent work in data gathering.
Participants: A total of 113 (male: 74, female: 39; 2013: 43 students; 2014: 70 students) sixth-year Japanese medical students responded to both parts of the questionnaire (Table 1).
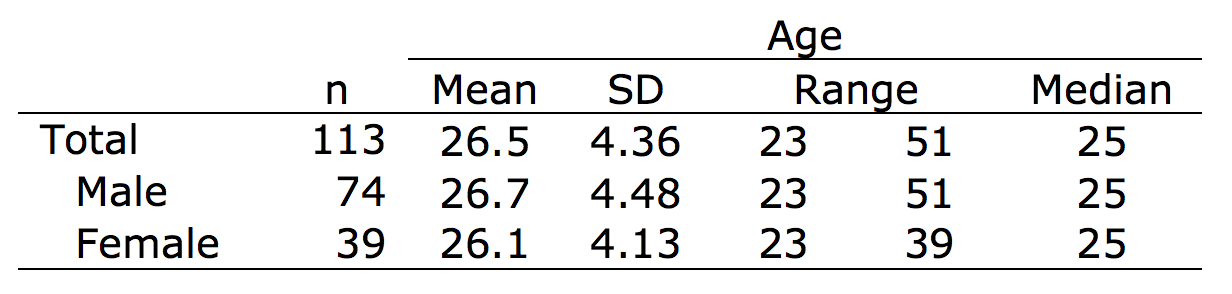
Table 1. Demographic characteristics of the participants.
The response rate was 52.8% (male 50.3%, female 58.2%) among the total of 214 students who were targeted.
RM encounters in formal clinical training courses and other situations.
- RM with positive and negative behaviors and actions
All and 91 students observed actions and behaviors of RM during formal clinical training and other opportunities, respectively, and 111 and 83 students observed positive and negative RM, respectively (Fig.1, Table 2). Two students only encountered negative RM.
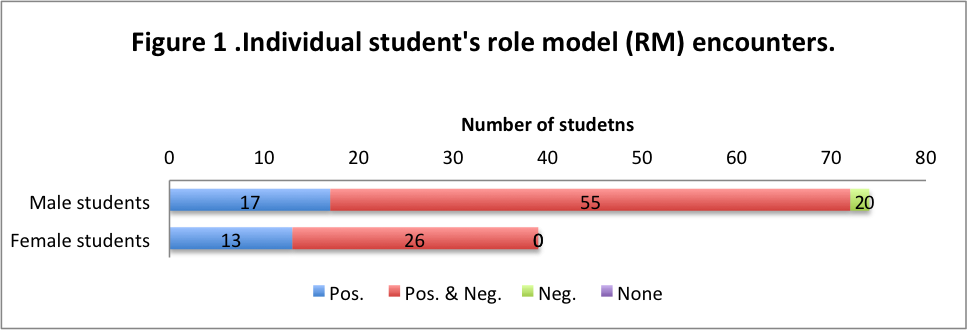
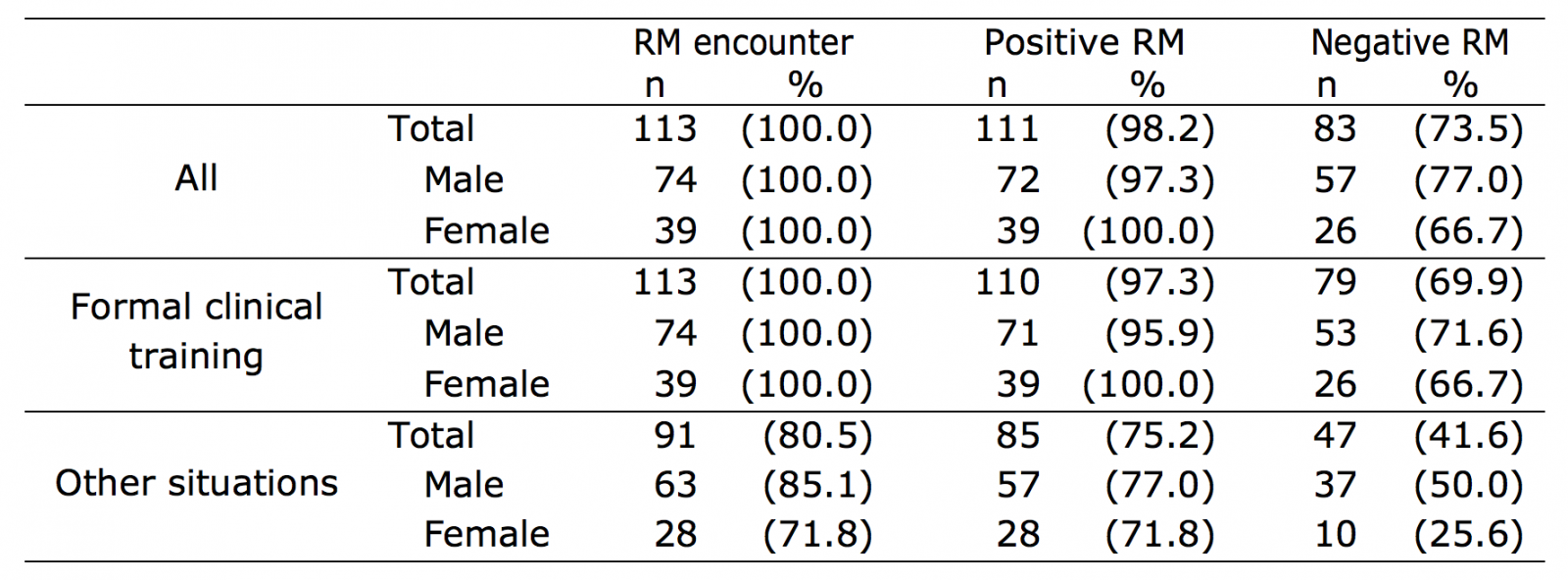
Table 2. Role model (RM) encounters in formal clinical training courses and other situations.
- Category of RM behaviors and actions
During formal training, students recognized positive and negative RM in terms of relationship with patients, clinical expertise, humanity, lifestyle, teaching, and community contribution (Fig. 2).
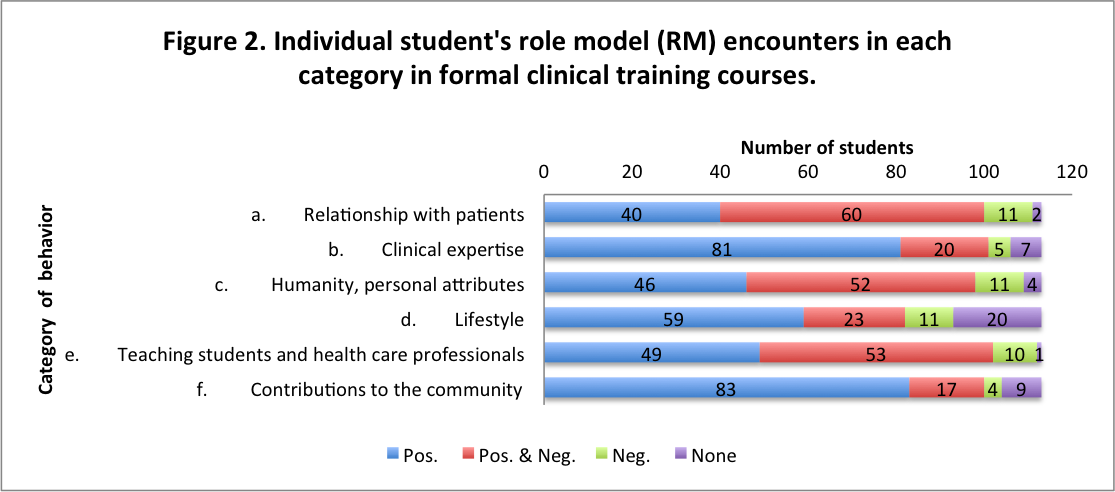
- Students' experieces and RM encounters
Frequent experiences of close clinical involvement and learning increased experiences of positive RM (Table3).
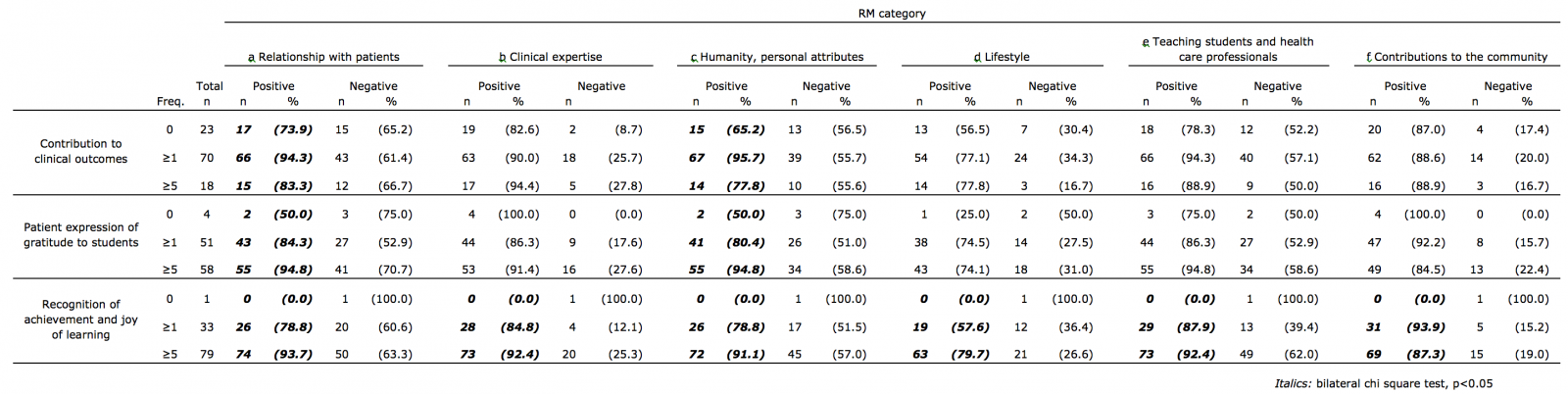
Table 3. Comparison of role model (RM) encounters with clinical and learning experiences in formal clinical courses.
Positive and negative RM encounters are compared among 3 different frequency groups (none, 1-4, 5 times or more) of specific clinical and learning experiences in formal clinical courses. Numbers and % of students who encountered RM in each category are indicated.

 Send Email
Send Email