


Theme
Simulation and Simulated Patients
Category
Simulation
INSTITUTION
Imperial College London

High fidelity simulation (HFS) training has been used for a number of years in medical schools to help teach medical students how to deal with situations occurring in acute and emergency medicine. Undergraduate students who have had training using HFS in the acutely ill patient have found the experience a `valuable addition’1 to their learning.
Obstetrics and Gynaecology foundation doctors are trained, in part, using simulated patients. Medical students are not, however, yet given this opportunity.
The confidence of students significantly improved in decision making and recognising patients in immediate danger. These areas may have improved most with HFS because students have less exposure to them during their rotation. This is supported by the raw data that shows students are less confident in these two areas before HFS than in the other domains that confidence was assessed in. A larger study is required to explore this further.
We propose embedding HFS into the undergraduate O&G curriculum to improve confidence in decision making and ability to recognise patients in immediate danger since these are necessary skills required by junior doctors.
The aim was to assess whether teaching with a simulated patient improved confidence in situation awareness, history taking, decision making and knowing when senior help is required. The confidence levels of eleven students were measured using a five-point Likert scale questionnaire before and after a HFS training session comprising an acute ectopic pregnancy.
.png)
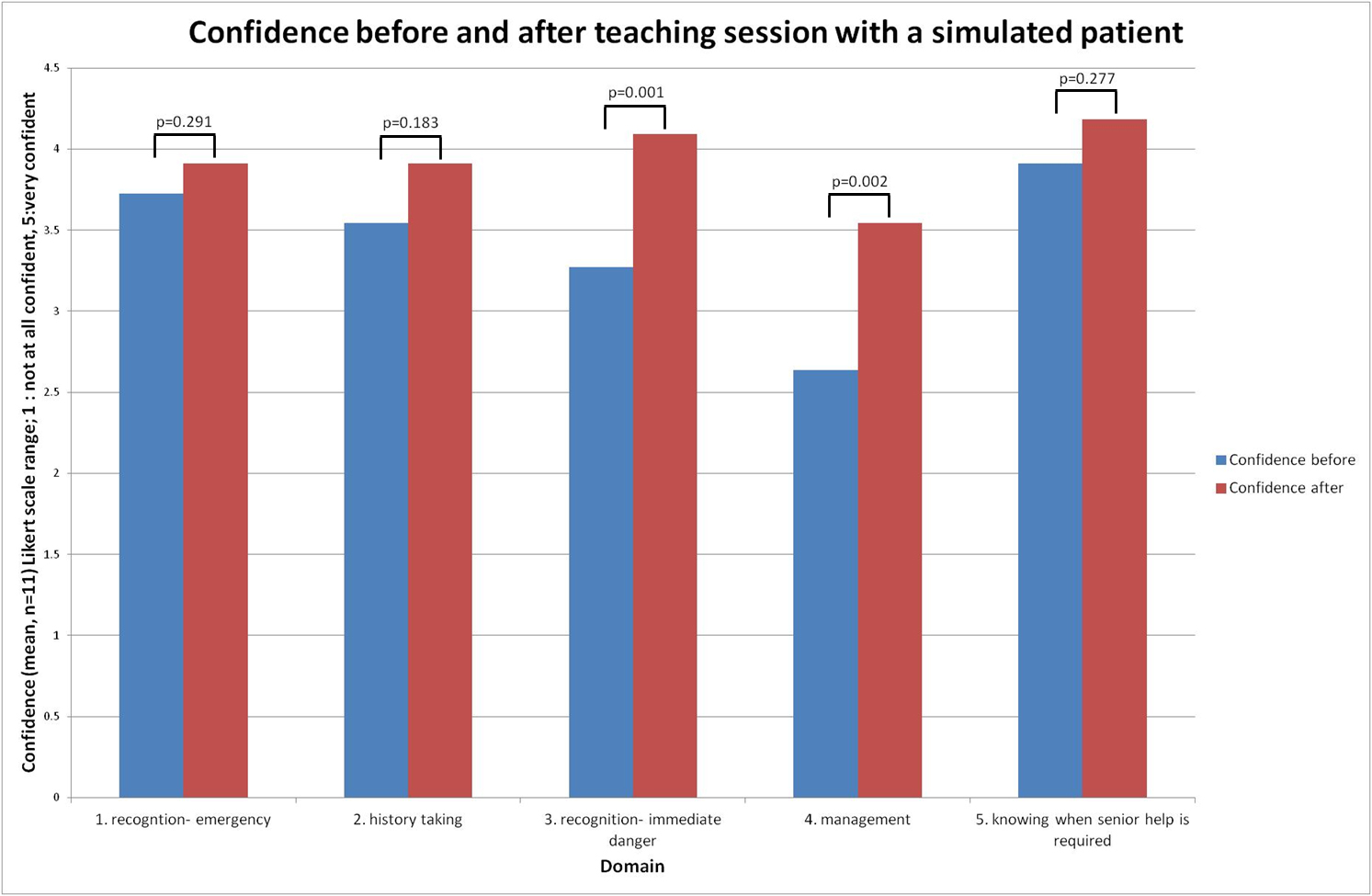 T-tests were carried out on the mean scores of the Likert-scale before and after HFS to determine any significant change in confidence. Click 'more detail' to see enlarged graph.
T-tests were carried out on the mean scores of the Likert-scale before and after HFS to determine any significant change in confidence. Click 'more detail' to see enlarged graph.
Dr. Roger Sharpe, Director of Medical Education, Northwick Park Hospital
Dr. Colin Mason, Research Fellow, Northwick Park Hospital
Dr. James Budge, Foundation Year 1, Ealing Hospital
1. Macdowell, J. (2006) The assessment and treatment of the acutely ill patient—the role of the patient simulator as a teaching tool in the undergraduate programme, Medical Teacher, 28(4): 326-9
2. Paskins, Z; Peile, E. (2010) Final year medical students' views on simulated-based teaching: a comparison with the Best Evidence Medical Education Systematic Review, Medical Teacher, 32(7): 569-77
3. Hansen, M. (2008) Versatile, Immersive, Creative and Dynamic Virtual 3-D Healthcare Learning Environments: A Review of the Literature Journal of Medical Internet Research, 10 (3):e26
 Send Email
Send Email