


Theme
International Medical Education
Category
General
INSTITUTION


Figure 6: Certificates at the end of the course
1) Teaching in an international setting has challenges but can be extremely effective and is a great opportunity to share skills and knowledge.
2) The change in attitudes towards mental health among the future medical profession is reassuring and highlights the need for on-going work in this area
3) This project should be extended through on-going e-teaching and also utilized in other areas where there is stigma associated with mental health and limited mental health resources
The Tropical Health and Education Trust (THET)1 is an international development organisation providing medical education and training in healthcare in developing countries2
King’s THET Somaliland Partnership (KTSP) began working in Somaliland (Figure 1) in 20033 and the mental health group started in 2007. There have been 12 trips prior to the trip in December 2011 8
Somaliland is an unrecognised independent state in Northern Somalia4 Somaliland has a population of 3.5 million and high numbers of internally displaced people5
There is no data for Somaliland, but in Somalia, mortality rates are high and there is a newly recognised high prevalence of mental health problems
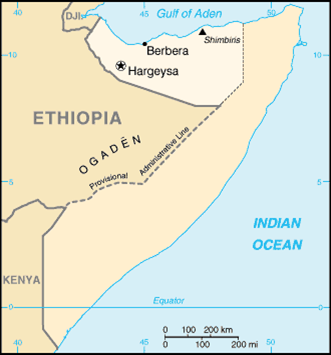
Figure 1: Map of Somaliland
Mental Health in Somaliland
One in three Somali’s has been affected by some kind of mental illness; a higher prevalence than other low-income, war-torn countries6
Khat is thought to be related to mental health problems.

Figure 2: Khat
In Hargeisa 21% of households care for at least one family member with a severe mental problem7,8
There are only two public inpatient psychiatric units in Somaliland8
There are no psychiatrists in Somaliland. Stigma and negative attitudes towards mental health are a major problem especially as these views extend among the medical profession
Preparation
• As a junior doctor, this trip followed involvement in a online e-teaching programme called medicineafrica
• After being selected to teach I was prepared by THET for the trip to Somaliland and given support throughout
• I was involved in developing the curriculum for the course and the teaching timetable for the course and led half of the sessions under the supervision of consultant psychiatrist, Dr Whitwell
• Due to technical limitations the lectures prepared in advance could not be accessed in Somaliland so I had to start from scratch when I arrived to re work my material.

Figure 3: Teaching by OSCE practice and role play
Content
• The experience comprised a two week international psychiatry course for final year medical students in Somaliland (in December 2011).
• Questionnaires completed before and after the course by students explored attitudes towards mental health (APT-30 and KTSP own questionnaire)
• Teaching was based in Hargesia Group Hospital
• The teaching including ward based group work; patient interaction, small group work, role play, case based discussions, OSCE practice.

Figure 4: A ward in Hargeisa Group Hospital
• MCQ and OSCE exam had to be passed at the end of the course for the students to progress through their final year
• Delivered with consideration of cultural and language barriers
1) Teaching psychiatry in Somaliland was a very worthwhile experience for a junior doctor to learn of the barriers faced by medics when attempting to address and treat mental health problems, and work together to overcome them.
2) It was valuable to develop my own teaching, management, presentation and communication skills and bring them back to the UK
3) Opportunities to share knowledge and mentor other doctors was an extremely rewarding experience and highlights the numerous benefits that can be gained from such international collaborations.
4) The course we delivered has hopefully inspired a new generation of doctors in Somaliland to work together to eliminate stigma towards mental health and be equipped to identify and treat these problems.
Quotes from students post-course:
"This course gave me the chance to learn how to approach mentally ill people"
"Every person in the medical field needs to know psychiatry”
"I'm one of the students who would like to be psychiatrist"
"Please come back and teach us more about psychiatry"
I would like to thank King's College London, and THET for sponsoring the trips. Many thanks to Professor John Rees (King's College London) for sponsoring this conference and supporting the work of this partnership.


Figure 5: Sitting the final exam
All students (n=38) passed the course; developing awareness and understanding of psychiatry.
Significant (p<0.05) improvement in attitudes (assessed with pre and post course KTSP questionnaires) towards mental health following our teaching course
14.7% of Somaliland final year medical students were planning on specialising in psychiatry by the end of the course
When compared to a similar sized group (n= 42) of UK taught final year medical students completing the same questionnaire, more Somaliland students were planning for a career in psychiatry than UK students.
Many of the students are now planning to pursue a career in psychiatry and hope to help those with mental illness, educate families and aim to eradicate the stigma associated with mental health problems in Somaliland
1 Parry, E. and V. Parry (1998). "Training for health care in developing countries: the work of the Tropical Health and Education Trust." Med Educ 32(6): 630-635.2http://www.thet.org/ (Accessed 18/6/12)3 http://www.thet.org/healthlinks/kings-thet-somaliland-partnership-ktsp/ (Accessed 18/6/12) 4 http://www.nytimes.com/2006/06/05/world/africa/05somaliland.html?_r=1 (Accessed 18/6/12)5 Bryden M (ed): Rebuilding Somaliland: Issues and Possibilities. Lawrenceville, NJ, and Asmara, Eritrea, Red Sea Press, 2005 6 http://www.who.int/hac/crises/som/somalia_mental_health/en/index.html (Accessed 18/6/12)7 Odenwald M, Neuner F, Schauer M, et al: Khat use as risk factor for psychotic disorders: a cross-sectional and case-control study in Somalia. BMC Medicine 3:5, 2005 8 Syed Sheriff, R. J., A. F. Baraco, et al. (2010). "Public-academic partnerships: Improving human resource provision for mental health in Somaliland." Psychiatr Serv 61(3): 225-227.
 Send Email
Send Email